Pelvic Floor Exercises
July 25, 2013 12:00 pm
What are the pelvic floor muscles?
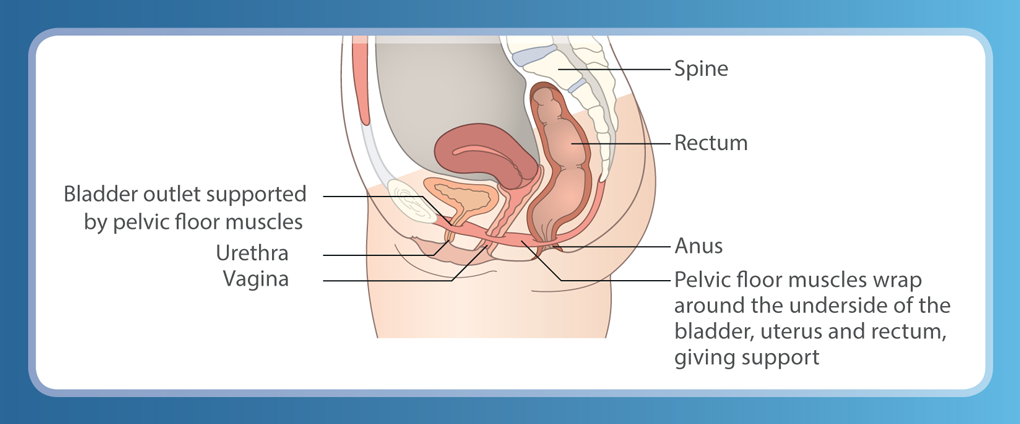
The pelvic floor muscles are a group of muscles that wrap around the underside of the bladder and rectum. Your doctor may advise that you strengthen your pelvic floor muscles:
- If you develop stress incontinence. Stress incontinence is when urine leaks when there is a sudden extra pressure (‘stress’) on the bladder. Urine tends to leak most when you cough, laugh, or when you exercise (like jump or run). Strengthening the pelvic floor muscles can often cure stress incontinence.
- After childbirth. The common reason for the pelvic floor muscles to become weakened is childbirth. If you do pelvic floor muscle exercises after childbirth, it may prevent stress incontinence developing later in life.
In addition, some people feel that having strong pelvic floor muscles heightens the pleasure when having sex.
Pelvic floor exercises are useful to prevent and/or cure stress incontinence; particularly for women who have had children.
Doing the exercises
- You need to do the exercises every day.
- Sit, stand or lie with your knees slightly apart. Slowly tighten your pelvic floor muscles under the bladder as hard as you can. Hold to the count of five, then relax. Repeat at least five times. These are called slow pull-ups.
- Then do the same exercise quickly for a second or two. Repeat at least five times. These are called fast pull-ups.
- Keep repeating the five slow pull-ups and fast pull-ups for five minutes.
- Aim to do the above exercises for about five minutes at least three times a day, and preferably 6-10 times a day.
- Ideally, do each five minute bout of exercise in different positions. That is, sometimes when sitting, sometimes when standing, and sometimes when lying down.
- As the muscles become stronger, increase the length of time you hold each slow pull-up. You are doing well if you can hold each slow pull-up for a count of 10 (about 10 seconds).
- Do not squeeze other muscles at the same time as you squeeze your pelvic floor muscles. For example, do not use any muscles in your back, thighs, or buttocks.
- In addition to the times you set aside to do the exercises, try to get into the habit of doing exercises whilst going about everyday life. For example, when answering the phone, washing up, etc.
- After several weeks the muscles will start to feel stronger. You may find you can squeeze the pelvic floor muscles for much longer without the muscles feeling tired.
It takes time, effort and practice to become good at these exercises. It is advised that you do them for at least three months to start with. You should begin to see benefi ts after a few weeks.
However, it often takes 8-20 weeks for most improvement to occur. After this time you may be cured of stress incontinence. If you are not sure that you are doing the correct exercise, ask a doctor, physiotherapist or continence advisor for advice.
If possible, continue exercising as a part of everyday life for the rest of your life to stop the problem recurring. Once incontinence has gone, you may only need to do 1-2 five minute bouts of exercise each day to keep the pelvic floor muscles strong and toned up, and incontinence away.
Pelvic floor exercises if you do not have incontinence
The type of exercises are exactly the same. If you are not used to pelvic floor exercises then perhaps do the exercises as often as described opposite for the first three months or so. This will strengthen up the pelvic floor muscles.
Thereafter, a five minute spell of exercises once or twice a day should keep the muscles strong and toned up, which may help to prevent incontinence from developing in later life.
Other ways of exercising pelvic fl oor muscles
Sometimes a continence advisor or physiotherapist will advise extra methods if you are having problems or need some extra help performing the pelvic floor exercises. These are in addition to the exercises described earlier. For example:
- Electrical stimulation. Sometimes a special electrical device is used to stimulate the pelvic floor muscles with the aim of making them contract and become stronger.
- Biofeedback. This is a technique to help you make sure that you exercise the correct muscles. For this, a physiotherapist or continence advisor inserts a small device into your vagina when you are doing the exercises. When you squeeze the right muscles, the device makes a noise (or some other signal such as a display on a computer screen) to let you know that you are squeezing the correct muscles.
- Vaginal cones. These are small plastic cones that you put inside your vagina for about 15 minutes, twice a day. The cones come in a set of different weights. At first, the lightest cone is used. You need to use your pelvic floor muscles to hold the cone in place. So, it helps you to exercise your pelvic floor muscles. Once you can hold onto the lightest one comfortably, you move up to the next weight, and so on.
- Other devices. There are various other devices that are sold to help with pelvic floor exercises. Basically, they all rely on placing the device inside the vagina with the aim of helping the pelvic muscles to exercise and squeeze. There is little research evidence to show how well these devices work. It is best to get advice from a continence advisor or physiotherapist before using any. One general point is that if you use one, it should be in addition to, not instead of, the standard pelvic floor exercises described above.
References
Urinary incontinence: the management of urinary incontinence in women , NICE (2006).
Dumoulin C, Hay-Smith J; Pelvic floor muscle training versus no treatment for urinary incontinence in women. A Cochrane systematic review . Eur J Phys Rehabil Med. 2008 Mar;44(1):47-63. (abstract)
Hay-Smith J, Morkved S, Fairbrother KA, et al; Pelvic floor muscle training for prevention and treatment of urinary and faecal incontinence in antenatal and postnatal women. Cochrane Database Syst Rev. 2008 Oct 8;(4):CD007471. (abstract)
Lagro-Janssen TL, Debruyne FM, Smits AJ, et al; Controlled trial of pelvic floor exercises in the treatment of urinary stress incontinence in general practice. Br J Gen Pract. 1991 Nov;41(352):445-9. (abstract)
Bo K, Talseth T, Holme I; Single blind, randomised controlled trial of pelvic floor exercises, electrical stimulation, vaginal cones, and no treatment in management of genuine stress incontinence in women. BMJ. 1999 Feb 20;318(7182): 487-93. (abstract)
Shamliyan TA, Kane RL, Wyman J, et al; Systematic review: randomized, controlled trials of nonsurgical treatments for urinary incontinence in women. Ann Intern Med. 2008 Mar 18;148(6):459-73. Epub 2008 Feb 11. (abstract)